
Jimmy Kimmel had joked the First Lady was an 'expectant widow' days before White House Correspondents’ Dinner
The latest national and international news stories that will inform you, make you laugh and make you think.

Jimmy Kimmel had joked the First Lady was an 'expectant widow' days before White House Correspondents’ Dinner
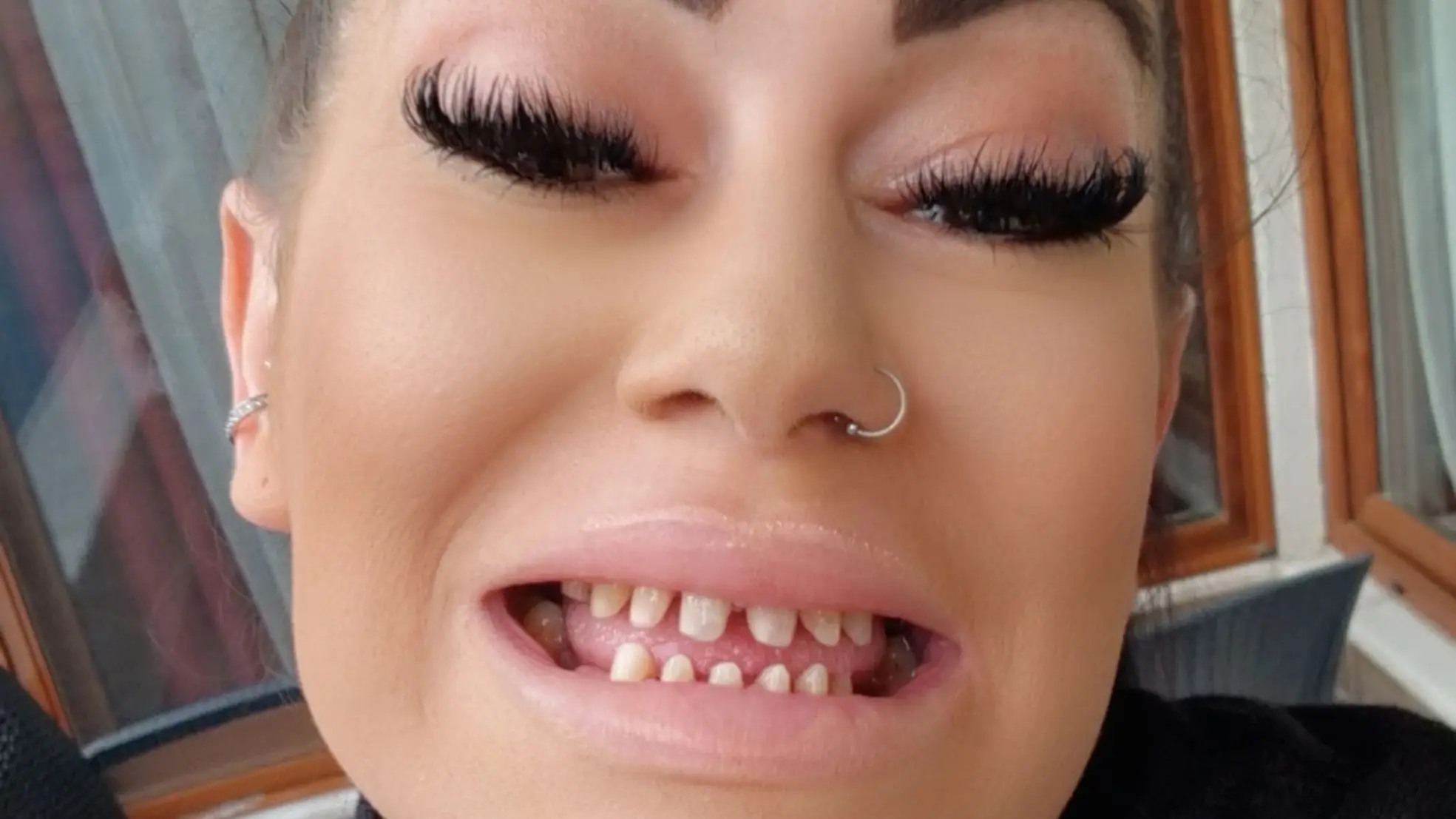
Jackie Lynn suffered a life-threatening blood infection after having new teeth fitted in Turkey

Activist Emma Smart said she'd been subjected to a 'witch hunt' after 'liberating' the marine animal

They're finally going to step into the ring against each other
breaking